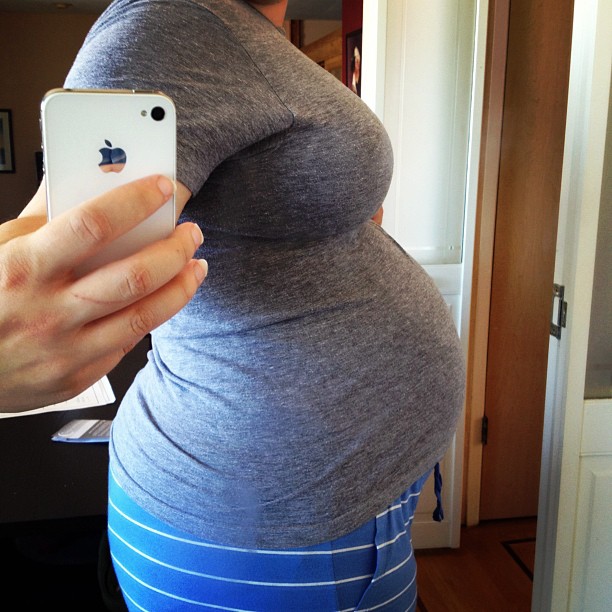
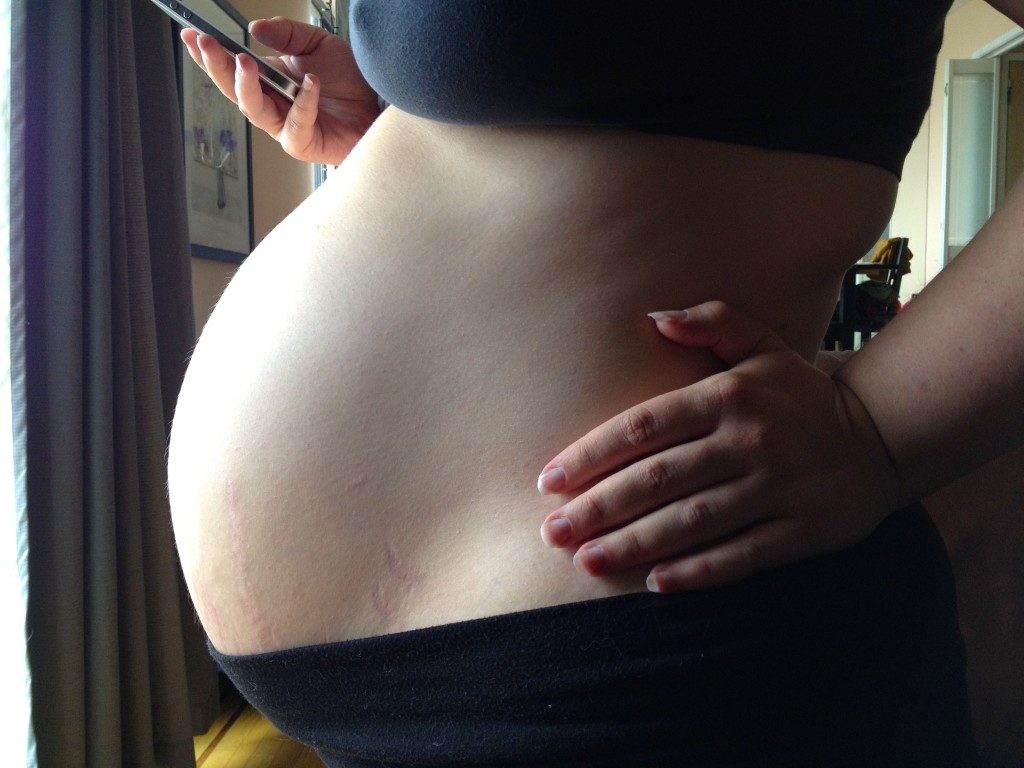
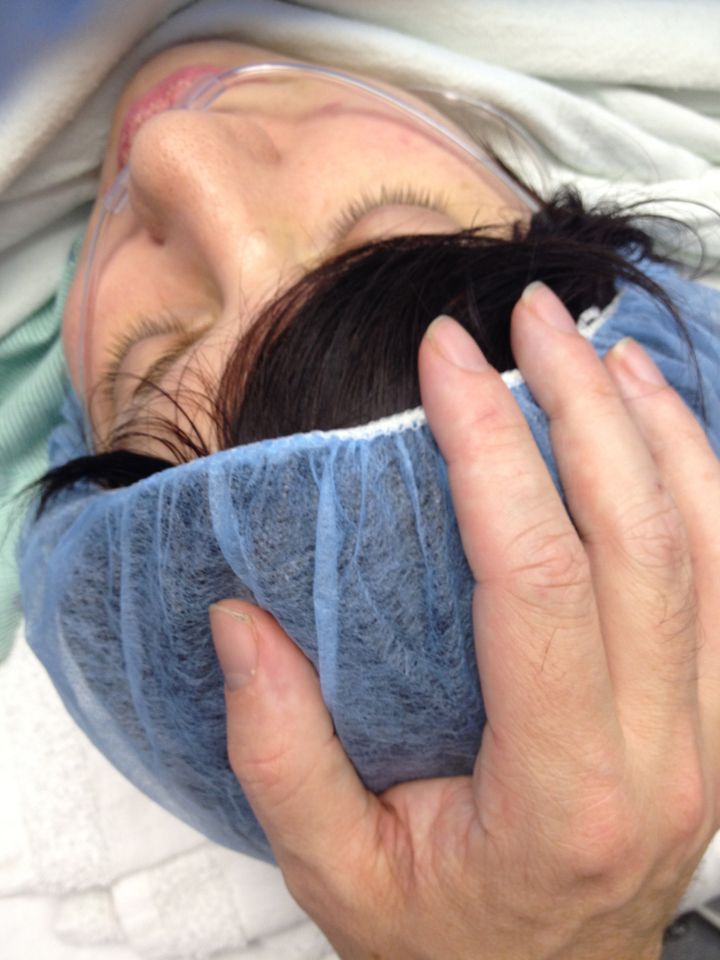
We pulled up to the hospital at 6:30am Sunday morning. The Daddy threw a “WOMAN IN LABOR” sign on the dash and ran for a wheelchair. We made our way up to the fifteenth floor. Contractions in the hallway, contractions in the elevator. At least the hospital was mostly empty at that hour.
He wheeled me to the nurses station and as he was checking us in, I had a powerful contraction. I was still feeling it mostly in my back and rectum and sitting in the wheelchair was too painful. I didn’t wait to get checked in – I leapt out of the wheelchair toward waiting nurses and growled, “Get me in a room and give me drugs” and stormed down the hall, blood and fluid running down my legs, in the direction of open doors. The nurses raced ahead, led me to the delivery room and called the anesthesiologist.
Initial drama aside, the home-to-hospital transfer was flawless. Our midwife beat us there and was waiting with our records. I was in a room before The Daddy finished checking in and I had fentanyl administered and an epidural on the way within ten minutes.
The anesthesiologist came right away but we had to wait out two contractions before the epidural was placed. I bit down so hard during the second that I started wondering if it’s possible to shatter your own teeth. I hoped that the fentanyl would take the edge off while waiting for the epidural but its most notable effect was making me hear voices every time I closed my eyes. Luckily after two contractions, there was a long enough break to get the epidural placed with no problems. Relief!
With pain controlled, reality set in – I was in a hospital over 30 hours after my water had broken. Would they rush me into a c-section? Treat me poorly because we were a home birth transfer? I questioned our decision and wondered if I should’ve stayed home and found a way to deal with the excruciating pain. Logic gave way to fear and for a moment, I forgot about the other reason we transferred – the baby didn’t seem to be handling labor well. Those thoughts were interrupted by our nurse asking about our birth plan and someone checking my cervix.
My cervix wasn’t swollen. I was dilating again. Contractions had slowed and the baby seemed ok. My midwife acted as doula and the hospital staff were accepting of her being there – she had my prenatal charts, a labor flow chart, and was helpful in relaying our birth plan. A nurse quickly jotted down our birth plan and didn’t bat an eye at us declining all but one newborn procedure. The doctors were wonderful. They accepted everything we wanted and didn’t push us. They supported our vaginal birth goal and did everything they could to facilitate that. It was a shock and relief.
Pitocin was started to try and get regular contractions going again. I dilated quickly, the swelling was gone, and I started pushing. After a few pushes, the contractions spaced out and I fell asleep. I woke up a little while later to alarms and people rushing into the room. The baby’s heart rate dropped like it had at home, but it hadn’t recovered. A nurse shot terbutaline into my thigh to stop contractions and then flipped me on all fours (literally – the epidural made my left leg completely numb and I couldn’t move it at all) and rushed me to the OR for emergency surgery.
The Daddy was in the bathroom and had no idea what was happening when he walked out and they were wheeling me away. I was taken into the room alone, getting bits and pieces of what might be happening on our way down the hall. I was concerned for The Daddy and wondering if anyone had stayed behind to tell him what was going on. As soon as we got into the OR and they prepared to put me under, her heart rate went back up. Back to the delivery room, to try again.
Pitocin was restarted when the terbutaline wore off. The baby tolerated labor and pushing for awhile. Pushing was a relief; the pain went away and I felt like I was finally doing something productive. I pushed for four hours. I pushed her from -1 to +3, The Daddy saw her head and reported that she had tons of hair. We thought we were going to make it (apparently I was an “excellent pusher”). She was distressed again. Her heart rate took a very long time to recover. I don’t remember a lot of what followed. I know I got two more shots of terbutaline because the baby’s heart rate fell and didn’t come back up. I know they fiddled with my dose of pitocin. An alarm went off again. At some point, my epidural failed and I had to have another one put in. The second one failed, too. By this point, Sunday was ending. I was exhausted and scared for the baby and didn’t feel like I could go on. The hospital birth team came in. We talked options.
We were given three choices:
-Keep pushing with the understanding that another decel would mean emergency surgery where I’d be put under and The Daddy would not be allowed in the room.
-Try forceps and risk vaginal tearing, injury to the baby, and the possibility of it not working and needing a cesarean anyway.
-Have a c-section right away.
The hospital team left us to talk. I asked the midwife her opinion and if she thought forceps or surgery were warranted. She suspected a cord issue and thought it’d be best to get baby out quickly. After discussing with her and The Daddy, we decided forceps were worth a try and told the rest of the team.
The attending physician did a vaginal check and said there was no room for forceps. Our options were keep pushing or head to the OR. The hospital staff left the room again so we could talk. We decided to have the surgery. And with that, they wheeled me to the OR while The Daddy left to get scrubbed and changed so we could begin phase three.